 Conclusion: A lightweight, water-resistant, and ventilated cast can be designed and printed within 24-48 hours. 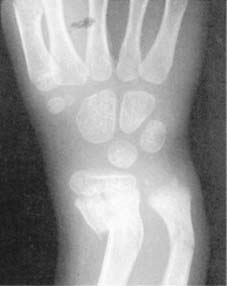
The human cadaver model study showed displacement in the models if a static load is placed on them. Three children with greenstick or buckle/torus fractures were successfully treated with 3D-printed casts. The pilot study showed it is feasible to treat a patient within 24 hours after admission to the ER. The casts could be printed within 24-48 hours. Results: The material tests showed PLA was the best material to print with Fused deposition modeling (FDM).ith a semi-automated design, printable casts were created. A final step was the human model cadaver study, where a static load was placed on the casts to see if the cast could prevent secondary displacement of the DRF in a cadaver model. A pilot study was conducted to assess three aspects of 3D casts treatment: the feasibility of the implementation of 3D-printed casts, the clinical outcomes, and patient experiences. A workflow was designed to test feasibility and implementation in the clinic. Material tests were conducted to select the most suitable design and material. Methods: Multiple sub-studies were performed. The aim was to investigate the feasibility of 3D printed casts, the implementation of 3D casts for the treatment of distal radius fractures, and to characterize the magnitude of fracture displacement during static load in human cadaver models with Colles fractures. Literature showed no consensus about the materials, printers, design, and implementation in the clinic for 3D-printed casts. 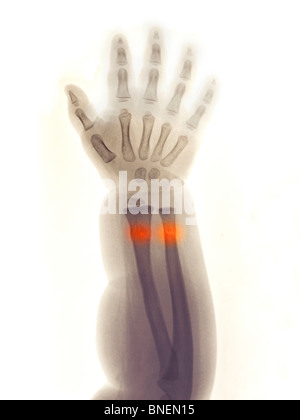
The 3D-printed cast could overcome these issues: they are lightweight, waterproof, open-latticed. Up to 30% of plaster casting leads to complications. Introduction: Distal radius fractures (DRF) are traditionally treated with plaster casts, which have disadvantages. A precise classification of fracture type at the time of diagnosis would identify a smaller subset of patients that require follow-up.Distal radius fracture management Using 3D printed, in-house design, production, and implementation of wrist cast/orthosis for the treatment of distal radius fractures. Complete fractures of the distal radius are uncommon in children, and highly unstable. Greenstick fractures are unstable and continue to displace after 2 weeks. īuckle fractures are stable and do not require follow-up. On average, the complete fractures displaced 9 degrees. The greenstick fractures displaced 5 degrees on average, and continued to displace after the first 2 weeks. 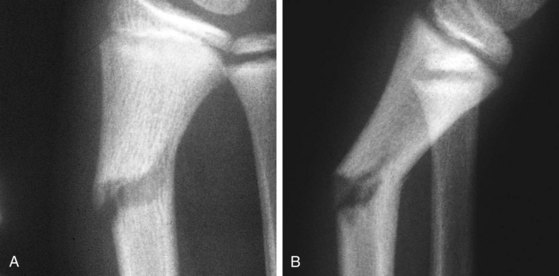
The lateral angulation of the buckle fractures did not change importantly throughout the treatment. The greenstick fractures had more complications than the buckle fractures. Only 1 of 311 follow-ups led to an active intervention. The fracture type was determined from the initial radiographs and the angulation on the lateral films was noted. The medical records of 305 distal radius fractures in patients aged less than 16 years treated at our institution in 2006 were reviewed, and any complications were noted. The stability of greenstick and buckle fractures of the distal radius was assessed by comparing the lateral angulation radiographically. We investigated the degree to which the follow-up visits reveal complications and lead to change in management. Numerous follow-up visits for wrist fractures in children are performed without therapeutic consequences. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
